
Comparing the effectiveness of fascia iliaca block with standard analgesia in neck of femur fractures in a district general hospital emergency department—a prospective study with review of literature
Introduction
As the demographic of the population changes to a greater prevalence of the elderly population the incidence of neck of femur fracture increases. In 2016, there was over 65,000 people aged 60 years and older that presented to hospitals in England, Wales and Northern Ireland (1) with hip fractures. This number is said to reach an incidence of 101,000 by the year 2020 (2). The total annual cost in the management of hip fractures is estimated to be more than £2 billion.
Pain has both physiological and psychological components. The pain following hip fractures has been linked to altered physiological states leading to the development (3) of delirium, depression and sleep disturbance, thereby highlighting the important of effective management from admission through to rehabilitation. Since the inception of fascia iliaca block (FIB), this has been widely used in all patients with confirmed neck of femur fractures unless there has contraindications.
With the ageing population, the prevalence of cognitive impairment in the population will also rise, with this the co-existing morbidities will also rise. With this the incidence of polypharmacy, the effective analgesia that can be provided in addition to the regular prescribed analgesia is somewhat limited.
Contraindications to having FIB include patient refusal, underlying cognitive impairment (procedure made complicated due to inability to stay still), underlying coagulopathy and if patient on oral anticoagulants as this would increase the chance of bleeding. The contraindications differ if the procedure is done via the landmark method or through ultrasound guidance. In our department the landmark method is used.
Methods
We had 2 distinct parameters that we measured in our Emergency department at University Hospital Ayr. The first parameter that we measured was the time to reassessment and the pain scores at reassessment, the RCEM guidance states that patients with severe pain need to be assessed within 60 min.
The second parameter was the analgesic effect that FIB had on pain relief. We used these values to perform a comparative analysis of the pain scores. We calculated the percentage change in the level of pain for both patients receiving FIB and those patients not suitable for FIB. A simple pain score tool was used, in which patients would denote their pain score from 0- no pain to 10-severe pain.
The Scottish standards of care for hip fracture [2016] (4) advises that patients with confirmed diagnosis of hip fracture should be transferred within 4 h to the acute orthopaedic receiving ward unless requiring essential medical interventions.
In our hip fracture ED proforma there is an allocated space for documenting the analgesia the patient has received. We underwent a trial to ascertain if the use of additional pain management stickers would be more effective than using our longstanding hip fracture proforma.
We found that the uptake of the stickers was patchy and at times of severe bed wait pressures, the uptake was limited. From the completed records, it was noted that there we were not meeting the 30 min target set by the RCEM for administration of analgesia for severe pain.
We reverted to use of our longstanding hip fracture proforma with clear instructions sent out to all clinicians that the pain scores and analgesia given need to be clearly documented. Whilst this was ongoing, our nursing staff were working on improving documentation of the time analgesia was given and amendments were made to the proforma.
We also carried out a study comparing the effectiveness of analgesia provided by standard pain management with the analgesia provided with FIB.
Results
The preliminary study included a small cohort of patients to assess how well the 2 parameters could be assessed.
The time for reassessment of pain score was average at 72 min. (Figure 1). This is approximately 12 min greater the RCEM guidance of 60 min. However, we noted that was a 43.4% improvement in pain score on reassessment.
In patients with low pain scores 1–3, the effective analgesia that FIBs can provide can be limited. However, the more important aspect to consider the duration of time that the analgesic relief that can be gained from FIBs. This is particularly important in reducing pre-operative analgesia and post-operative analgesia requirements as highlighted in the article.
FIBs
In the UK as part of the post graduate curriculum in the Foundation Training Programme in emergency medicine, the ability to perform FIBs are emphasized upon. In our department, the trainees on rotation and taught and assessed on their ability to perform FIBs and they develop a level of competency in performing this. Until recently this was a procedure performed by anaesthetists and orthopaedic surgeons. FIBs are the current recommendation for hip fractures unless there are any contraindications for this procedure.
The National Institute of Health and Care Excellence (NICE) recommends that simple analgesia should be used with FIBs used as an adjunct (5). In 2016 Callear et al. (6), evaluated the proportion of patients receiving FIB as well as the efficacy of these block with pre and post-operative opioid analgesia amongst other measures. The outcome from the study was noted that a single dose FIB given in the pre-operative period reduced both post-operative and the overall requirement of analgesia. An interesting fact to note is the reduction in the rates of delirium and length of hospital stay.
In a systematic analysis by Steenberg et al. (7) in the British Journal of Anaesthetics revealed a superior analgesic effect of FIB when compared with opioids. It also noted that patients that received FIB has lower pre-operative analgesia requirement and longer time to first request for analgesia.
The studies also indicated that with any movement, in patients receiving FIB the pain scores were reasonably lower than other modes of analgesia. Studies comparing analgesia effect of FIB with NSAIDs demonstrated a significant greater analgesic effect with FIB compared with NSAIDs.
Table 1 highlights that in 11 out of 25 patients (44%) of patients there was no change or improvement in the pain score. However, it’s worth noting that in 6 out of these 11 patients (54.5%) the pain at reassessment was 0. The readers may agree that FIBs should still be indicated in these 6 patients as means of longer acting pain relief. This is especially the case if the patients were not operated on immediately. From the overall perspective there was a percentage improvement in pain post FIB 41.8%
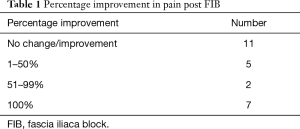
Full table
The average to having a FIB done was noted to be 132 min, the RCEM does not have an exact time frame to have procedure done. On certain occasions the procedure was performed within the hour, however in certain cases there was delay in the procedure being done due to various factors.
From the 42 patients in our study 9 patients (21.4%) refused to have procedure done, according to the RCEM guidance this is an absolute contraindication to the procedure. Performing FIBS using the landmark process, patients being on oral anticoagulants is a relative contraindication, this constituted another 4 patients (9.5%).
Identified potential scopes for improvement in future studies
We identified that there were certain flaws in our method which could be looked in the future studies. The main flaw was pain assessment in patients with cognitive impairment where a verbal response was not reliable.
As our readers may be aware that in all Emergency Departments in the National Health Trusts (NHS) have a 4-hour target within which the patient presenting to the Emergency Department needs to be assessed, treated and subsequently referred/discharged.
In our Emergency Department we have a 2-hour time target within which the assessment and preliminary treatment of patients with neck of femur fractures are carried out. We have a fast track system where having been assessed and stabilised they are admitted directly to our orthopaedic ward. If a hospital bed were to be made available on the trauma and orthopaedic ward, the patient would be treated and transferred to the ward within the 2-hour period. This would make data collection with regards to the analgesic effect of FIB difficult to collate.
As highlighted in our study the average time to having the FIB performed was 132 min which would breach our 2-time target, however this was noted to be multifactorial. We propose performing the FIBs soon after triage in any suspected neck of femur fractures unless there are any contraindications in our future studies. We could then possibly assess the further analgesia requirement if our FIBs did not work.
We also suggest the level of pain experienced by patient may be influenced by the level of background analgesia and other factors (Table 2). Within our patient study group, co-existent painful conditions such as osteoarthritis and inflammatory arthropathies were prevalent. These patients were invariably on a wide range of analgesia with a significant proportion of patients on long term analgesia. We hope the readers will appreciate the complexities involved in considering the aforementioned issue.

Full table
Conclusions
FIBs provide effect analgesia in the vast majority of patients with neck of femur fractures. Through this study we have highlighted the importance of early and effective analgesia in patients with significant pain scores leading to patient wellbeing. We have also highlighted a number of measures that could be undertaken to further improvement patient experience and eventually lead to improvement in patient recovery.
Acknowledgments
None.
Footnote
Conflicts of Interest: The author has no conflicts of interest to declare.
Ethical Statement: The author is accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. There was no patient identifiable information used in the data collection and subsequent data processing. There was no identifiable need for ethical approval in the processing and publication of this article.
References
- The National Hip Fracture Database. Available online: https://www.nhfd.co.uk/
- British Geriatrics Society. The care of patients with fragility fractures. British Orthopaedic Association, 2007:4.
- The management of chronic pain in older persons: AGS panel on chronic pain in older persons: American geriatrics society. J Am Geriatr Soc 1998;46:635-51. [Crossref] [PubMed]
- Scottish Standards of Care for Hip Fracture Patients. 2016. Available online: http://www.shfa.scot.nhs.uk/_docs/20161109_SSC_for_Hip_Fracture_Patients.pdf
- National Clinical Guideline Centre. The management of hip fractures in adults. London: National Clinical Guideline Centre, 2014:7-9.
- Callear J, Shah K. Analgesia in hip fractures. Do fascia-iliac blocks make any difference? BMJ Qual Improv Rep 2016. [Crossref] [PubMed]
- Steenberg J, Møller AM. Systematic review of the effects of fascia iliaca compartment block on hip fracture patients before operation. Br J Anaesth 2018;120:1368-80. [Crossref] [PubMed]
Cite this article as: Chowdhury D. Comparing the effectiveness of fascia iliaca block with standard analgesia in neck of femur fractures in a district general hospital emergency department—a prospective study with review of literature. J Emerg Crit Care Med 2019;3:43.



