
Artificial intelligence in emergency medicine
Introduction
Artificial intelligence (AI) in medicine has a long history (1). AI has been an active subfield of computer science for more than 60 years, while medicine is even a much older field, which can trace back to thousands of years. Researchers from both AI and medicine communities have been interacting to create novel solutions for better patient care and enabling more efficient healthcare systems (2,3). Collaborations between both communities were either technology-driven or problem-driven. In technology-driven research, innovations are mainly the development and validation of new AI algorithms for selected clinical problems where the algorithms are generic and not necessary to be optimal in solving real-world problems. In problem-driven research, AI algorithms are customized to fit in specific clinical problems to deliver the best solutions, which however may not have excellent generalizability to other problems. Over the years, the gap between technology-driven and problem-driven research is getting smaller and smaller.
Development of an efficient informatics infrastructure has been instrumental in the field of AI in medicine. The advancement of computational power and storage capability enables processing massive amount of healthcare data with sophisticated AI algorithms. Large-scale image understanding and real-time patient monitoring data analysis become reality. Boosted by the computing power of the latest graphics processing unit (GPU), techniques such as deep learning (4) has gained fame in handling complex clinical data including medical images (5,6) and electronic health records (7). AI solutions have been traditionally popular in intensive care (8) and cardiology (9). Handelman and colleagues (10) have well described the state-of-the-art of AI in medicine and its future directions. However, due to the width of medicine and the breadth of AI, it is not possible to describe every innovation in the interactions between AI and medicine. In this paper, we aim to summarize several AI applications in emergency medicine. We categorize these studies into three domains, namely AI in predictive modeling, AI in patient monitoring, and AI in emergency department (ED) operations. Subsequently, we will elaborate the discussions on AI for emergency medicine and make concluding remarks.
AI in predictive modeling
One natural application of AI in medicine is predictive modeling. Numerous AI systems have been built to predict risk of disease and adverse outcomes. Notably, in emergency medicine, AI has been well explored for creating predictive models. Graham et al. (11) used AI algorithms and data mining tools to predict hospital admissions with patient data collected at the ED, where logistic regression, decision trees and gradient boosted machines (GBM) were implemented. Hu et al. (12) developed a real-time web-based tool to assess the risk of future ED visit where multiple data mining and machine learning methods were adopted for prediction. This study demonstrated that data from not only hospital or ED but also outpatient clinics could be valuable in enabling population-based risk assessment where AI played an important role. In the study by Lee et al. (13), a clinical decision tool was proposed to predict patients who will return to the ED within 72 hours. This tool could enable ED staffs and administrators to use patient specific values to assess the probability of ED revisit within 72 hours, which provides an opportunity for improving care and offering additional guidance to reduce ED readmissions.
Among various AI tools and algorithms, artificial neural network is one of the most popular. The study by Walsh and colleagues (14) showed the feasibility of using artificial neural network ensembles to predict ED disposition for infants and toddlers with bronchiolitis, although the prediction of length of stay was found not good. Bektaş et al. (15) developed a predictive model using artificial neural network for predicting craniocervical junction injury in trauma patients. Harrison and Kennedy (16) proposed a predictive model of acute coronary syndromes using artificial neural network and clinical data at the ED presentation. Jenny et al. (17) assessed predictability of routinely collected variables for mortality and acute morbidity by building models with 17 statistical and AI methods including neural networks. Another example is Eken et al. (18) where artificial neural network and genetic algorithms (a metaheuristic inspired by the process of natural selection) were adopted to predict renal colic in the emergency settings.
The availability of massive amount of data in the electronic health records enables the use of large, complex dataset for predictive modeling. However, traditional logistic regression will not be feasible when there are more independent variables than observations (9). To address this issue, variable selection is effective and efficient. Liu et al. (19) created a ranking algorithm to select a few variables to achieve comparable predictive performance with the full set of variables in assessing the risk of major adverse cardiac events for ED patients with chest pain. Taylor and colleagues (20) used established random forest algorithm to rank variables according to their computed importance and demonstrated the power of AI and machine learning over clinical scores in predicting in-patient mortality for ED sepsis patients.
AI in patient monitoring
Facilitated with advanced sensor technologies and the rise in computing power, continuous acquisition and analysis of large-scale patient physiological data are no long in imaginations. Curtis et al. (21) presented an integrated wireless system to monitor unattended patients in the ED. In this study, a prototype of scalable medical alert response technology (SMART) system was piloted and a small-scale deployment was conducted. In a recent study by Clifton et al. (22), an integrated patient monitoring system was developed and validated in large-scale in the ED. The integrated system interfaced to a peer-to-peer network of bed-side monitors and hand-held PDAs. The authors compared two early warning systems (EWS) that developed on the integrated system and traditional manual system. The reported large clinical trial also evaluated automatic methods for assessment of patients based on electronic health records augmented with AI techniques. Generally, integrated patient monitoring systems are paired with AI components for assistive decision making. There were other research studies investigating the use of AI tools for handling physiological data such as electrocardiography in the emergency setting (23,24).
AI in ED operations
Resource planning and crowd management are important tasks in the ED. In Sun et al. (25), the authors used time series analysis technique called the autoregressive integrated moving average (ARIMA) to develop models for prediction of workload at the ED. Their research showed evidence on using forecasting models for the arrangement of staff roster and resource planning. In the study by Jones and Evans (26), the authors addressed ED overcrowding in terms of evaluating the impact of physician staffing configurations by developing an agent based simulation tool. The feasibility of such a tool has been evaluated at a single hospital ED.
Diagnostic decision tools are essential in the ED to screen and stratify patients. Haug et al. (27) proposed a system for diagnostic modeling, which could potentially automate the creation of diagnostic decision support applications. The system was validated in the ED and has demonstrated feasibility of extending it to other departments. Similarly, Grigull and Lechner (28) used data mining techniques to support diagnostic decisions in a pediatric emergency department.
AI and machine learning tools have also been widely adopted for various operational purposes in the ED. For example, Zmiri et al. (29) implemented several data mining methods including Naïve Bayes and C4.5 algorithm for triaging ED patients by measuring their severity grades. Comparably, Goto et al. (30) used several machine learning approaches to predict ED dispositions to facilitate the triage of asthma and chronic obstructive pulmonary disease (COPD) patients. Yadav and colleagues (31,32) proposed automated outcome classification of ED computed tomography (CT) reports for both adult and pediatric patients, where hybrid natural language processing (NLP) and machine learning systems were built. NLP played an important role in another study (33) where the authors proposed an automated subjective, objective, assessment, plan (SOAP) framework for emergency department reports.
Discussion
The amount of complex health data including images, texts, videos, genomic sequences and structured electronic health records, continues to grow. The needs of AI and machine learning are increasing to analyze these heterogeneous data as traditional biostatistical solutions are unable to handle. AI has been proven effective and useful in augmenting physicians in terms of enhancing operational efficiency for healthcare systems. As summarized in Table 1, the studies investigated earlier have shown evidence on how ED physicians and the department could benefit from AI and machine learning technologies. Many researches on using AI for emergency medicine have been well reviewed in (34) and (35). Our paper aims to analyze this field from different perspectives, by categorizing AI applications in emergency medicine into three domains, namely predictive modeling, patient monitoring, and ED operations. Apparently, there are more AI applications beyond the above-mentioned areas. For instance, Ni et al. (36) developed an automated system to prescreen clinical trial eligibility in the ED to improve the efficiency of patient identification.
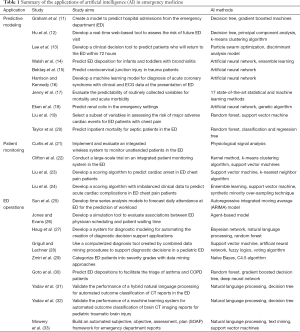
Full table
So far, the intersection of AI and emergency medicine is under-developed. Both areas have sophisticated development and rich individual sub-fields. The ED sees a big variety of patients and thus provides many opportunities to treat and study heterogeneous patient cohorts, such as trauma, sepsis, cardiovascular, among others. Likewise, AI has broad fields that study robotics, image, audio, video, text, genomics, and various applications. Given the fact that increasing number of technological innovations are available for real-time patient monitoring and system integrations, AI will play an instrumental role in the ED, in areas such as intelligent monitoring, clinical outcome prediction, and resource planning.
In this paper, we are not aiming to elaborate AI and machine learning algorithms, which has been done in many review articles (8-10); instead we emphasize on several specific AI applications in emergency medicine. We further categorize these applications into three domains, to which we believe most AI applications in the ED would belong. Even though AI solutions seem to be effective and useful in many applications, they are not universal. Customizations of AI algorithms to fit into specific clinical problems and needs are essential. This demands close collaborations between ED physicians and computer scientists. Therefore, building a culture and platform of knowledge sharing is a crucial step moving towards widespread adoption of AI and machine learning in emergency medicine.
Acknowledgements
None.
Footnote
Conflicts of Interest: The authors have no conflicts of interest to declare.
References
- Coiera EW. Artificial intelligence in medicine: the challenges ahead. J Am Med Inform Assoc 1996;3:363-6. [Crossref] [PubMed]
- Jiang F, Jiang Y, Zhi H, et al. Artificial intelligence in healthcare: past, present and future. Stroke Vasc Neurol 2017;2:230-43. [Crossref] [PubMed]
- Miller DD, Brown EW. Artificial Intelligence in Medical Practice: The Question to the Answer? Am J Med 2018;131:129-33. [Crossref] [PubMed]
- LeCun Y, Bengio Y, Hinton G. Deep learning. Nature 2015;521:436-44. [Crossref] [PubMed]
- Ting DSW, Cheung CY, Lim G, et al. Development and Validation of a Deep Learning System for Diabetic Retinopathy and Related Eye Diseases Using Retinal Images From Multiethnic Populations With Diabetes. JAMA 2017;318:2211-23. [Crossref] [PubMed]
- Litjens G, Kooi T, Bejnordi BE, et al. A survey on deep learning in medical image analysis. Medical Image Analysis 2017;42:60-88. [Crossref] [PubMed]
- Rajkomar A, Oren E, Chen K, et al. Scalable and accurate deep learning with electronic health records. npj Digital Medicine 2018;1:18.
- Hanson CW 3rd, Marshall BE. Artificial intelligence applications in the intensive care unit. Crit Care Med 2001;29:427-35. [Crossref] [PubMed]
- Johnson KW, Torres Soto J, Glicksberg BS, et al. Artificial Intelligence in Cardiology. J Am Coll Cardiol 2018;71:2668-79. [Crossref] [PubMed]
- Handelman GS, Kok HK, Chandra RV, et al. eDoctor: Machine learning and the future of medicine. J Intern Med 2018. [Epub ahead of print]. [Crossref] [PubMed]
- Graham B, Bond R, Quinn M, et al. Using Data Mining to Predict Hospital Admissions From the Emergency Department. IEEE Access 2018;6:10458-69.
- Hu Z, Jin B, Shin AY, et al. Real-time web-based assessment of total population risk of future emergency department utilization: statewide prospective active case finding study. Interact J Med Res 2015;4. [Crossref] [PubMed]
- Lee EK, Yuan F, Hirsh DA, et al. A clinical decision tool for predicting patient care characteristics: patients returning within 72 hours in the emergency department. AMIA Annu Symp Proc 2012;2012:495-504. [PubMed]
- Walsh P, Cunningham P, Rothenberg SJ, et al. An artificial neural network ensemble to predict disposition and length of stay in children presenting with bronchiolitis. Eur J Emerg Med 2004;11:259-64. [Crossref] [PubMed]
- Bektaş F, Eken C, Soyuncu S, et al. Artificial neural network in predicting craniocervical junction injury: an alternative approach to trauma patients. Eur J Emerg Med 2008;15:318-23. [Crossref] [PubMed]
- Harrison RF, Kennedy RL. Artificial neural network models for prediction of acute coronary syndromes using clinical data from the time of presentation. Ann Emerg Med 2005;46:431-9. [Crossref] [PubMed]
- Jenny MA, Hertwig R, Ackermann S, et al. Are Mortality and Acute Morbidity in Patients Presenting With Nonspecific Complaints Predictable Using Routine Variables? Acad Emerg Med 2015;22:1155-63. [Crossref] [PubMed]
- Eken C, Bilge U, Kartal M, et al. Artificial neural network, genetic algorithm, and logistic regression applications for predicting renal colic in emergency settings. Int J Emerg Med 2009;2:99-105. [Crossref] [PubMed]
- Liu N, Koh ZX, Goh J, et al. Prediction of adverse cardiac events in emergency department patients with chest pain using machine learning for variable selection. BMC Med Inform Decis Mak 2014;14:75. [Crossref] [PubMed]
- Taylor RA, Pare JR, Venkatesh AK, et al. Prediction of In-hospital Mortality in Emergency Department Patients With Sepsis: A Local Big Data-Driven, Machine Learning Approach. Acad Emerg Med 2016;23:269-78. [Crossref] [PubMed]
- Curtis DW, Pino EJ, Bailey JM, et al. SMART--an integrated wireless system for monitoring unattended patients. J Am Med Inform Assoc 2008;15:44-53. [Crossref] [PubMed]
- Clifton DA, Wong D, Clifton L, et al. A large-scale clinical validation of an integrated monitoring system in the emergency department. IEEE J Biomed Health Inform 2013;17:835-42. [Crossref] [PubMed]
- Liu N, Lin Z, Cao J, et al. An intelligent scoring system and its application to cardiac arrest prediction. IEEE Trans Inf Technol Biomed 2012;16:1324-31. [Crossref] [PubMed]
- Liu N, Koh ZX, Chua ECP, et al. Risk scoring for prediction of acute cardiac complications from imbalanced clinical data. IEEE J Biomed Health Inform 2014;18:1894-902. [Crossref] [PubMed]
- Sun Y, Heng BH, Seow YT, et al. Forecasting daily attendances at an emergency department to aid resource planning. BMC Emerg Med 2009;9:1. [Crossref] [PubMed]
- Jones SS, Evans RS. An agent based simulation tool for scheduling emergency department physicians. AMIA Annu Symp Proc 2008.338-42. [PubMed]
- Haug PJ, Ferraro JP, Holmen J, et al. An ontology-driven, diagnostic modeling system. J Am Med Inform Assoc 2013;20:e102-10. [Crossref] [PubMed]
- Grigull L, Lechner WM. Supporting diagnostic decisions using hybrid and complementary data mining applications: a pilot study in the pediatric emergency department. Pediatr Res 2012;71:725-31. [Crossref] [PubMed]
- Zmiri D, Shahar Y, Taieb-Maimon M. Classification of patients by severity grades during triage in the emergency department using data mining methods. J Eval Clin Pract 2012;18:378-88. [Crossref] [PubMed]
- Goto T, Camargo CA Jr, Faridi MK, et al. Machine learning approaches for predicting disposition of asthma and COPD exacerbations in the ED. Am J Emerg Med 2018;36:1650-4. [Crossref] [PubMed]
- Yadav K, Sarioglu E, Smith M, et al. Automated outcome classification of emergency department computed tomography imaging reports. Acad Emerg Med 2013;20:848-54. [Crossref] [PubMed]
- Yadav K, Sarioglu E, Choi HA, et al. Automated Outcome Classification of Computed Tomography Imaging Reports for Pediatric Traumatic Brain Injury. Acad Emerg Med 2016;23:171-8. [Crossref] [PubMed]
- Mowery D, Wiebe J, Visweswaran S, et al. Building an automated SOAP classifier for emergency department reports. J Biomed Inform 2012;45:71-81. [Crossref] [PubMed]
- Berlyand Y, Raja AS, Dorner SC, et al. How artificial intelligence could transform emergency department operations. Am J Emerg Med 2018;36:1515-7. [Crossref] [PubMed]
- Stewart J, Sprivulis P, Dwivedi G. Artificial intelligence and machine learning in emergency medicine. Emerg Med Australas 2018. [Epub ahead of print]. [Crossref] [PubMed]
- Ni Y, Kennebeck S, Dexheimer JW, et al. Automated clinical trial eligibility prescreening: increasing the efficiency of patient identification for clinical trials in the emergency department. J Am Med Inform Assoc 2015;22:166-78. [Crossref] [PubMed]
Cite this article as: Liu N, Zhang Z, Ho AF, Ong ME. Artificial intelligence in emergency medicine. J Emerg Crit Care Med 2018;2:82.


