Torsion of a wandering spleen in a young thalassemic patient
A 19-year-old Asian, thalassemic female presented with abdominal pain for 3 days. The pain started in the supraumbilical area and migrated to the suprapubic area, with nausea, anorexia, and diarrhea. On pelvic examination, purulent discharge was found with cervical motion tenderness. She was treated as a pelvic inflammatory disease. The abdominal examination was not performed. Two days later, she revisited with central abdominal pain, anorexia, and vomiting, without either diarrhea or fever. Vaginal discharge or tenderness of cervix was not presented. Tenderness at a para-umbilical area without guarding but rebound tenderness was noted on abdominal examination.
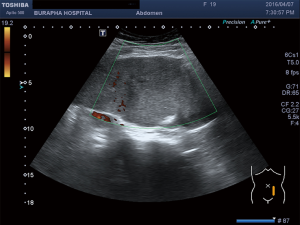
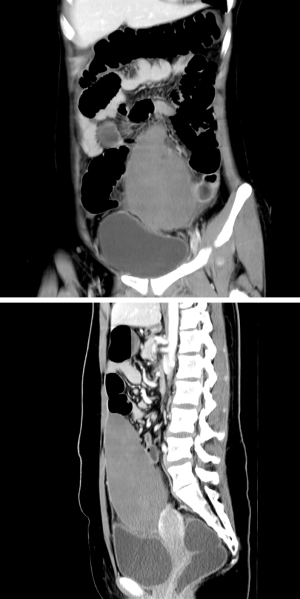
Increased white cell count of 25,960 cells/mm3 with neutrophil predominate (87%) was found. Greyscale ultrasonography (US) revealed abnormally located enlarged spleen at left lower quadrant. Color Doppler US (CDUS) showed flow in the vascular pedicle but no flow in the spleen parenchyma (Figure 1). Contrast-enhanced computed tomography (CT) of the abdomen demonstrated inferomedially displaced spleen to mid of abdomen with non-enhanced parenchyma (Figure 2). Whirled sign was observed at a splenic vascular pedicle. Wandering spleen with torsion was suggested.
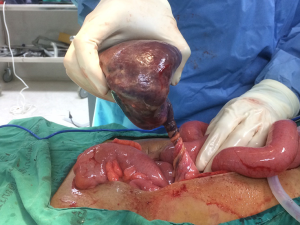
Emergency laparotomy revealed wandering of spleen located at the midline of the abdomen with torsion of vessels (Figure 3). Splenectomy was performed. Histological examination indicated acute hemorrhagic infarction of the spleen.
Wandering spleen is a rare anatomical abnormality due to the congenital anomaly or from acquired conditions such as splenomegaly, connective tissue disease, or abdominal trauma. The major complication is torsion of splenic hilum, which may be acute, intermittent or chronic. Wandering spleen usually presents between 20 and 40 years of age, being more common in females. Clinical symptoms and signs are usually not helpful in diagnosis. The US can be used and this entity should be suspected when the US cannot demonstrate spleen in the normal location. Whirled sign from contrast-enhanced CT is specific for torsion.
Acknowledgements
The authors are grateful to Faculty of Medicine Burapha University for all supports.
Footnote
Conflicts of Interest: The authors have no conflicts of interest to declare.
Informed Consent: Written informed consent was obtained from the patient for publication of this manuscript and any accompanying images.
Cite this article as: Limchareon S, Chaivanit T, Hirunpattarasilp W. Torsion of a wandering spleen in a young thalassemic patient. J Emerg Crit Care Med 2018;2:61.